Home
Women’s Health Knowledge Center
Which Birth Control Method Is Best? A Detailed Comparison of Pills, Injections, Implants, and IUDs
The question women ask most often is
“Which birth control method is best?”
There is no single best answer
but there is a method that is “right for each person’s body and lifestyle.”
At Femily Wellness Clinic
many patients are undecided between 4 main methods, including:
Birth control pills
Intrauterine device (IUD)
Contraceptive implant
Contraceptive injection
This article explains them in detail and straightforwardly
1️⃣ Birth control pills (oral contraceptive pill)

How it works
Estrogen + progestin
prevents ovulation and thins the uterine lining
Effectiveness
When used correctly: >99%
In real life (with occasional missed or late pills): about 91%
Advantages
More regular menstrual cycles
Reduces menstrual pain
May improve acne in some people
Disadvantages
Must be taken every day
Nausea during the first few weeks
Risk of forgetting to take it
Some medical conditions mean it should not be used
Suitable for
Women who are disciplined and want to control their menstrual cycle
2️⃣ Intrauterine device (Intrauterine Device: IUD)

There are 2 types:
Copper IUD (hormone-free)
Hormonal IUD
Effectiveness 99%
Advantages
No need to remember it every day
Lasts 3–10 years
Fertility returns quickly after removal
Disadvantages
Must be inserted and removed by a doctor
Some people have spotting during the first few months
Suitable for
Women who want long-term contraception
The hormonal IUD is especially good at reducing heavy periods
3️⃣ Contraceptive implant (Implant Contraception)

Inserted under the skin of the upper arm
continuously releases progestin hormone
Effectiveness
99% (very high)
Advantages
Lasts 3-5 years
Ideal for people who are forgetful
Disadvantages
Spotting is common
Must be inserted and removed by a doctor
Suitable for
For busy working adults, the implant is a very popular option because it is convenient and reliable
4️⃣ Contraceptive injection
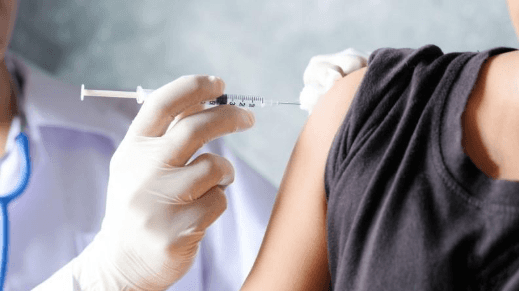
Contraceptive injection delivers hormones into the body through the muscle
to prevent ovulation and thin the uterine lining
There are 2 commonly used main types:
Injection every 1 month
Injection every 3 months
🔹 Monthly injection (Combined Injectable)
Contains
estrogen + progestin
Highlights
Menstrual cycles often remain close to normal
Less spotting than the 3-month injection
Hormones are similar to combined oral contraceptive pills
Points to consider
Requires a monthly injection
Not recommended for people at risk of blood clots, such as heavy smokers or those over 35 with other risk factors
🔹 Every-3-month injection (DMPA – Progestin only)
Contains only progestin
Highlights
No estrogen needed
Suitable for people who cannot use combined hormonal contraception
Only 4 injections per year (every 3 months)
Points to consider
Periods may stop
Spotting is common during the first few months
After stopping, it may take several months for ovulation to return
If used long term, bone health should be assessed as appropriate
According to the guidelines of
World Health Organization
and American College of Obstetricians and Gynecologists
long-term DMPA use is acceptable in people without contraindications, but patients should be counseled about its effects on bone density before making a decision
How to choose
In working adults who want regular periods
the monthly injection is often more satisfying
But for those who are breastfeeding or cannot use estrogen
the 3-month injection is the better option
The most important thing is to explain “abnormal bleeding in the early period” clearly
because many people stop using it out of concern, even though it is a common side effect that usually improves over time
Summary of choices
Want regular periods → Monthly injection
Cannot use estrogen / breastfeeding → Every-3-month injection
Do not want frequent periods → Every-3-month injection
The choice should be made with a doctor to assess individual risk factors
Comparison point | Monthly injection | Every-3-month injection |
Hormone type | Estrogen + progestin | Progestin only |
Injection frequency | Every 1 month | Every 3 months |
Menstrual cycle | Usually comes every month as normal | May become lighter or stop |
Spotting | Less common | Common in the first few months |
Who it suits | People who want regular periods | People who cannot use estrogen |
Return of ovulation after stopping | Faster | May take several months |
So which one is “best”?
Method | Effectiveness | Duration | Need to remember often? |
Pill | ~91–99% | Every day | Yes |
IUD | >99% | 3–10 years | No |
Implant | >99% | 3-5 years | No |
Injection | ~94% | 1,3 months | Every 1,3 months |
No method is the best it should be assessed based on:
Age
Underlying medical conditions
Whether the person smokes
When they want to have children
Whether they have menstrual problems
According to the guidelines of
American College of Obstetricians and Gynecologists
Long-Acting Reversible Contraception (LARC), such as IUDs and implants, is recommended as a first-line option for women without contraindications
Frequently asked questions
Does the implant cause weight gain?
Some people may gain a little weight, but not everyone
Does IUD insertion hurt?
You may feel brief cramping; it only takes a few minutes
After stopping injections, is pregnancy delayed?
It may take 6–12 months for the menstrual cycle to return to normal
What should I do if I forget one pill?
It depends on which week of the pack you are in; please read the label or consult a doctor
Summary
If you want maximum convenience → implant or IUD
If you want menstrual cycle control → pills
If you do not want estrogen → injections, implant, or IUD
The most appropriate choice should be made with guidance from a specialist doctor
Written by
Dr. Vichdet Vichchulda
Obstetrics and Gynecology Specialist
Currently pursuing subspecialty training in Maternal-Fetal Medicine at King Chulalongkorn Memorial Hospital
Research published in the International Journal of Transgender Health
References
American College of Obstetricians and Gynecologists (ACOG). Long-Acting Reversible Contraception Practice Bulletin.
World Health Organization. Medical eligibility criteria for contraceptive use.
Williams Obstetrics, 26th Edition.